Mental health providers across the USA are seeing a sharp rise in patient demand, but many practices continue to struggle with one critical issue—accurate Medicare reimbursement. From psychotherapy sessions and psychiatric evaluations to telehealth documentation and coding compliance, even minor billing mistakes can lead to delayed payments, denials, or compliance risks.
That’s why understanding the process of billing Medicare for mental health services has become essential for therapists, psychiatrists, psychologists, counseling centers, and behavioral health clinics. Medicare billing rules are constantly evolving, and providers who fail to stay updated often experience revenue leakage without realizing it.
This guide explores the key aspects of Medicare mental health billing, common mistakes providers make, and how specialized billing support can improve operational efficiency and financial performance.
Why Medicare Billing for Mental Health Services Is So Complex
Behavioral health billing is significantly different from general medical billing. Mental health claims involve detailed documentation requirements, strict coding standards, therapy time tracking, authorization rules, and payer-specific reimbursement policies.
For Medicare patients, providers must also comply with:
- Coverage limitations
- Medical necessity guidelines
- Telehealth billing rules
- CPT and ICD-10 coding accuracy
- Timely filing requirements
- Modifier usage standards
Because of these complexities, many practices now rely on mental health insurance billing services to reduce administrative burden and improve reimbursement accuracy.
A qualified mental health billing specialist understands the nuances of behavioral health coding and helps providers avoid costly errors that can interrupt cash flow.
Common Challenges in Billing Medicare for Mental Health Services
Even experienced practices face recurring billing issues. The most common problems include:
Incorrect CPT Code Selection
Mental health coding depends heavily on session duration, service type, and provider credentials. Choosing the wrong CPT code can result in underpayments or denials.
Examples include:
- Psychotherapy sessions
- Medication management
- Psychiatric diagnostic evaluations
- Group therapy
- Family counseling sessions
Many providers partner with a mental health billing and coding company to ensure coding accuracy and payer compliance.
Documentation Deficiencies
Medicare requires clear evidence of medical necessity. Missing treatment plans, incomplete progress notes, or insufficient session documentation can trigger audits and denials.
This is where mental health medical billing services become valuable. Billing experts often review documentation before claim submission to identify gaps early.
Telehealth Billing Confusion
Telepsychiatry and virtual therapy sessions continue to expand across the USA, but billing requirements frequently change. Providers must use correct modifiers, POS codes, and telehealth-specific documentation standards.
A trusted mental health billing services agency can help practices stay updated with evolving Medicare telehealth guidelines.
High Claim Denial Rates
Behavioral health practices commonly face denials due to:
- Eligibility verification failures
- Authorization issues
- Duplicate claims
- Incorrect modifiers
- Missing provider credentials
Working with a mental health billing consultant helps practices identify denial patterns and implement corrective workflows.
Key Medicare Mental Health Services That Require Accurate Billing
Behavioral health providers bill Medicare for a wide range of services. Some of the most frequently reimbursed services include:
Psychiatric Diagnostic Evaluations
Initial patient assessments require detailed documentation and accurate diagnosis coding. Incorrect coding can delay payment or trigger medical review.
Individual Psychotherapy
Session duration determines the CPT code selection. Providers must document start and stop times clearly.
Group Therapy Sessions
Medicare has strict requirements regarding participation, treatment goals, and session structure.
Medication Management
Psychiatrists and qualified providers must ensure documentation aligns with evaluation and management coding guidelines.
Telehealth Counseling
Virtual therapy reimbursement depends on payer-specific rules, provider eligibility, and proper modifier usage.
Because these services require precision, many clinics choose to outsource mental health billing services to experienced professionals who specialize in behavioral health reimbursement.
Why More Providers Are Choosing Outsourced Mental Health Billing
Mental health practices often operate with lean administrative teams. Handling patient care, scheduling, insurance verification, coding, appeals, and collections internally can overwhelm staff.
As a result, many organizations now prefer outsourced mental health billing models to improve efficiency and reduce operational stress.
Benefits of Outsourcing Include:
Improved Claim Accuracy
Experienced billing professionals understand behavioral health coding rules and Medicare requirements.
Faster Reimbursements
Clean claims reduce payment delays and improve cash flow consistency.
Reduced Administrative Burden
Providers can focus more on patient care rather than insurance follow-ups.
Better Denial Management
A professional mental health billing agency tracks denials, identifies root causes, and manages appeals effectively.
Regulatory Compliance Support
Billing specialists stay updated on Medicare policy changes and compliance standards.
Choosing the best mental health billing agency often helps practices scale operations without expanding in-house billing teams.
What to Look for in a Mental Health Billing Company
Not all billing providers specialize in behavioral health. Selecting the right partner requires careful evaluation.
Industry-Specific Experience
Choose a company that focuses specifically on behavioral health billing rather than general healthcare billing alone.
A reliable mental health billing provider should understand:
- Behavioral health CPT coding
- Medicare therapy limitations
- Psychiatric documentation requirements
- Telehealth reimbursement rules
Strong Denial Management Processes
An experienced mental health billing specialist should proactively track denied claims and implement correction strategies quickly.
Credentialing Support
Many billing delays happen because providers are improperly credentialed with Medicare or commercial payers.
Practices benefit significantly when a billing partner also offers credentialing services alongside billing operations.
Transparent Reporting
The best outsource mental health billing and coding company provides regular financial reporting, claim status visibility, and reimbursement analytics.
Scalable Solutions
As practices grow, billing systems must scale accordingly. A dependable mental health medical billing solution should support multi-provider practices, telehealth expansion, and multi-location operations.
How Mental Health Billing Impacts Revenue Cycle Performance
Revenue cycle management in behavioral health extends far beyond claim submission.
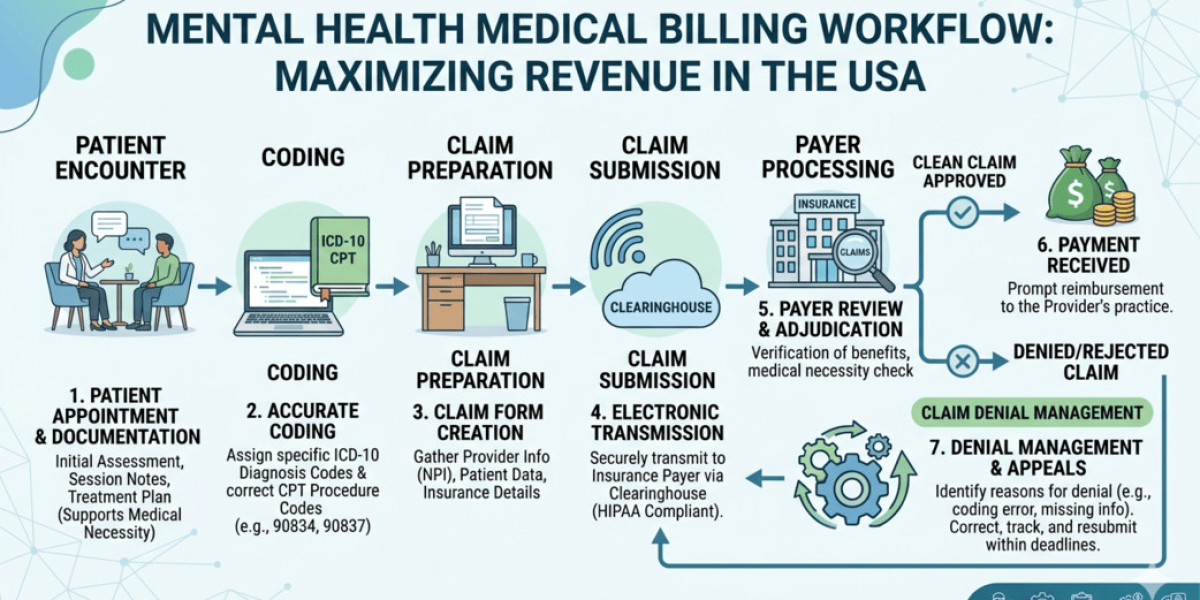
A successful billing workflow includes:
- Insurance verification
- Patient eligibility checks
- Accurate coding
- Timely claim submission
- Payment posting
- Denial management
- Appeals processing
- Patient collections
This is why many providers seek integrated revenue cycle management services rather than standalone billing support.
An optimized revenue cycle improves:
- Cash flow stability
- Claim approval rates
- Collection efficiency
- Operational productivity
- Patient financial transparency
For behavioral health organizations, strong billing operations directly influence long-term sustainability.
Real-World Example: How Billing Errors Affect Mental Health Practices
Consider a mid-sized therapy practice handling Medicare patients across multiple locations.
The clinic experienced:
- Frequent psychotherapy claim denials
- Delayed reimbursements
- High AR days
- Staff burnout from appeals processing
After partnering with a professional mental health billing company, the practice implemented:
- Accurate therapy coding workflows
- Automated eligibility verification
- Documentation audits
- Medicare compliance reviews
- Dedicated denial tracking
Within several months, the organization saw measurable improvements in reimbursement turnaround times and claim acceptance rates.
This scenario is increasingly common across the USA as behavioral health practices face rising administrative complexity.
The Growing Demand for Mental Health Billing Services in USA
Behavioral health awareness continues to grow nationwide, leading to increased patient volume and insurance claims.
At the same time, Medicare and commercial payers are tightening documentation requirements and reimbursement oversight.
This has created strong demand for:
- Mental health billing companies
- Billing services for mental health therapists
- Billing services for mental health providers
- Mental health insurance billing
- Mental health medical billing services outsourcing
Providers are recognizing that specialized billing support is no longer optional—it’s becoming essential for financial stability and compliance protection.
How Technology Is Changing Mental Health Medical Billing
Modern billing workflows rely heavily on automation and analytics.
Today’s advanced mental health medical billing solution platforms often include:
- Electronic claim scrubbing
- Automated eligibility verification
- Real-time claim tracking
- Telehealth billing integration
- AI-assisted denial analysis
- Revenue performance dashboards
However, technology alone is not enough. Human expertise still plays a major role in handling payer disputes, appeals, and behavioral health coding accuracy.
That’s why many providers combine technology with experienced mental health insurance billing services for stronger operational performance.
Why Integrated Billing and Coding Support Matters
Billing and coding errors are closely connected. A claim may fail simply because documentation does not fully support the selected code.
Working with teams that provide both medical billing services and medical coding services helps practices reduce inconsistencies across the reimbursement process.
Integrated medical billing and coding services also improve:
- Compliance accuracy
- Audit preparedness
- Reimbursement optimization
- Denial prevention
- Documentation consistency
Behavioral health practices that align billing, coding, and operational workflows generally experience better financial outcomes over time.
Supporting Practice Growth Through Strategic Revenue Management
Mental health providers today must balance clinical excellence with financial sustainability.
That requires more than basic claim submission. Practices increasingly need:
- Advanced revenue cycle management services
- Efficient payer communication
- Credentialing support
- Coding compliance monitoring
- Medicare reimbursement expertise
Organizations like 247 Medical Billing Services have become part of this growing industry shift by supporting healthcare providers with specialized billing workflows, coding accuracy, operational efficiency, and behavioral health reimbursement management.
As Medicare regulations evolve, partnering with experienced billing professionals can help providers reduce administrative pressure while maintaining a stronger focus on patient care.
Conclusion
Successfully billing Medicare for mental health services requires more than submitting claims. Providers must manage coding accuracy, documentation compliance, payer regulations, telehealth updates, and denial prevention simultaneously.
For many behavioral health practices across the USA, partnering with a specialized mental health billing agency offers a practical path toward improved reimbursements and operational efficiency.
Whether working with therapists, psychiatrists, counseling centers, or behavioral health clinics, experienced billing professionals help streamline workflows and reduce costly administrative challenges.
As the behavioral healthcare landscape continues to expand, practices that invest in specialized billing support, integrated medical billing services, accurate medical coding services, reliable revenue cycle management services, and effective credentialing services will be better positioned for long-term financial stability and sustainable growth.
FAQs
What is Medicare mental health billing?
Medicare mental health billing is the process of submitting claims for behavioral health services provided to Medicare beneficiaries. It includes psychotherapy billing, psychiatric evaluations, medication management, telehealth counseling, and related behavioral health services.
Why do mental health claims get denied frequently?
Mental health claims are often denied because of coding errors, missing documentation, authorization issues, incorrect modifiers, or eligibility verification problems.
Should therapists outsource mental health billing services?
Many therapy practices choose to outsource mental health billing services to improve claim accuracy, reduce administrative workload, and accelerate reimbursements.
What does a mental health billing specialist do?
A mental health billing specialist manages behavioral health claims, verifies insurance eligibility, handles coding compliance, submits claims, tracks denials, and follows up on reimbursements.
How do mental health billing companies improve revenue cycle performance?
Specialized billing companies improve claim accuracy, reduce denials, optimize reimbursement workflows, and strengthen overall revenue cycle efficiency for behavioral health practices.
Why are credentialing services important for mental health providers?
Proper credentialing services ensure providers are enrolled with Medicare and insurance payers correctly, helping prevent claim rejections and reimbursement delays.